Radiation Therapy
Radiation therapy services at the Veterinary Medical Center can treat many tumors with radiation therapy as well as occasionally benign tumor types or inflammatory conditions can be improved with radiation therapy.
What is Radiation Therapy?
Radiation therapy uses ionizing radiation to induce DNA damage within cancer cells, which ultimately results in cancer cell death. External beam radiation therapy using a linear accelerator (linac) is the most common type of radiation therapy, in which radiation beams are shaped to the aim at the pet’s tumor or surgical scar while avoiding as much normal tissue as possible. Most pets are anesthetized for each treatment and carefully positioned on a treatment couch. It is common for pets to need a CT scan in order to determine the extent of his/her tumor and to help devise a pet-specific radiation treatment plan. This may be needed even if a CT has been done previously for diagnosis or staging, in order to optimize your pet’s radiation plan. Pets are anesthetized for each treatment and we use fast-acting anesthesia protocols to ensure that each pet is alert and happy at home afterwards.
At the University of Minnesota, we house a Varian linear accelerator that uses both photons and electrons for treatment. We have additional advanced software to formulate treatment plans and have on-board imaging to ensure that the pet is properly positioned before treatment. Our clinical service is supported by the Department of Radiation Oncology at the Medical School. Their team of radiation oncologists, medical physicists, dosimetrists, and radiation therapists use similar software and equipment and their expertise helps to ensure we provide state-of-the-art care to our pet patients.
What types of tumors are commonly treated with radiation therapy?
Many tumors can be treated with radiation therapy. Occasionally benign tumor types or inflammatory conditions can be improved with radiation therapy, but most tumors amenable to radiation are malignant tumors including:
- Nasal tumors
- Brain tumors
- Spinal cord tumors
- Mast cell tumors
- Soft tissue sarcomas
- Injection site sarcomas
- Oral tumors including oral melanomas, squamous cell carcinomas, fibrosarcomas
- Anal sac (apocrine gland) tumors
- Bone tumors including osteosarcoma, chondrosarcoma, and multilobular osteochondrosarcoma
- Cardiac tumors
- Some lung and liver tumors
What type of radiation therapy is offered?
We offer several different types of radiation therapy, and the radiation oncology team including:
- Conformal radiation therapy (CRT)
- Image-guided radiation therapy (IGRT)
- Intensity modulated radiation therapy (IMRT)
- Stereotactic radiation therapy (SRT) or stereotactic body radiation therapy (SBRT)
- Electron therapy
- Plesiotherapy (Strontium)
Definitive-intent Radiation Therapy is typically administered to localized tumors with the primary goal of achieving long-term tumor control (often >1-3 years depending on the tumor) while minimizing any radiation injury to normal structures. It is most often used after surgery for incompletely excised tumor, where there is a reasonable risk of local tumor recurrence, but may be considered prior to surgery in some cases. Radiation therapy administered in this manner is often called definitive-intent radiation therapy (sometimes curative-intent) since it is aiming for the best chance at local tumor control. Most veterinary radiation patients undergoing definitive-intent radiation are treated over a 3-4 week period, with a small fraction (dose) of radiation administered daily through the week. Smaller doses of radiation are kinder to normal tissue that is near the tumor that is targeted. Traditionally, tumors are treated with 3D-conformal radiation therapy (CRT), which involves radiation beams that are “sculpted” around the tumor target based on CT images of each pet. Our machine is also capable of electron therapy, which is beneficial for some superficial tumors since this type of radiation does not deeply penetrate underlying tissues. Newer technology has enabled us to better target tumors with intensity-modulated radiation therapy (IMRT) as it can sculpt tightly around the tumor volume to decrease radiation dose to nearby tissue.
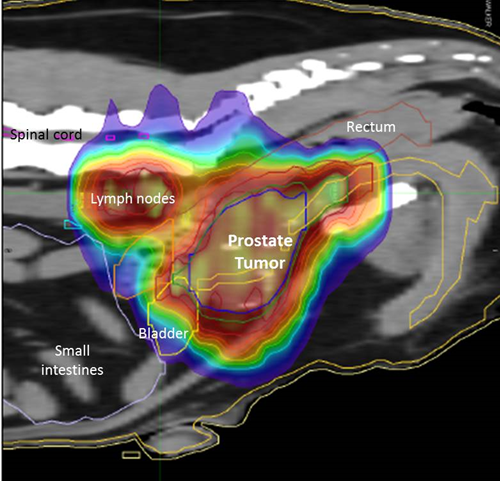
While we know the most about conventional radiation therapy, where radiation is given in small doses each day over several weeks, we are interested in investigating the use of higher doses of radiation that are administered less frequently. Stereotactic radiation therapy (SRT) or stereotactic body radiation therapy (SBRT) refers to the use of high doses of radiation given to macroscopic (visible) tumors in only 3-5 fractions. Currently, we do not know if this provides equal control to conventional RT for all tumor types, but it is an alternative option for owners wishing to consider a different approach. Not all dogs and cats are good candidates for this type of therapy.
Radiation plans are made specifically designed to each pet’s unique conformation, tumor shape, and tumor location. To do this, we perform a CT scan prior to radiation therapy in order to design a plan that targets the tumor and decreases dose to nearly normal tissues. Each CT plan is patient-specific since every dog has a slightly different conformation and features. Most CT scans are done 7-10 days prior to the planned starting day of radiation. We also use image-guidance (IGRT) for all patients that are prescribed IMRT or SBRT and most patients prescribed CRT to ensure that the patient is positioned properly. This ensures that the pet’s position at the time of treatment matches his or her position at the time of the CT scan, when the plan was designed.
Palliative radiation therapy has a different goal in that it may help relieve pain or improve function for pets with advanced cancer. These protocols can vary and may involve one treatment given weekly or treatments given over several days in a row. The duration of tumor control is shorter than with definitive-intent radiation therapy, however often helps to improve quality of life. Generally palliative radiation therapy is reserved for patients with advanced disease due to a higher risk of radiation damage to nearby normal tissue when compared to definitive protocols.
What is my pet's quality of life during radiation therapy?
Oncology teams make every effort to ensure that pets are comfortable and happy during treatment with excellent quality of life. With definitive-intent protocols, acute side effects in the irradiated site (such as radiation burn to the skin or mouth) may occur but are managed with supportive care and tend to heal quickly following treatment. The likelihood of acute effects is dependent on the location of the tumor and the radiation protocol. Late radiation effects may also occur, which are permanent irreversible changes to irradiated tissue that occur months to years following radiation therapy. Most late effects are mild and may include side effects such as coat color change (often to white) or permanent loss of hair in the irradiated skin. It is important to discuss potential side effects with your pet’s oncologist or radiation oncologist prior to therapy so that you know what to expect with treatment. Because palliative radiation therapy is administered with a different goal, acute side effects are rare but the potential for significant late effects is higher; however, as palliative radiation is typically reserved for advanced cancer, late effects are rare.